Introduction
Coronary artery blockage is one of the most common and dangerous heart conditions, representing a leading cause of heart attacks and sudden cardiac events.
It occurs when fats and cholesterol accumulate on the artery walls, gradually restricting blood flow to the heart muscle.
Early diagnosis and timely treatment can save lives and prevent serious complications.
In this article, we’ll discuss the symptoms of coronary artery blockage, how to detect it early, and explain the difference between cardiac catheterization and stent placement—two key treatment methods.
What Is Coronary Artery Blockage?
The coronary arteries are responsible for supplying oxygen-rich blood to the heart muscle.
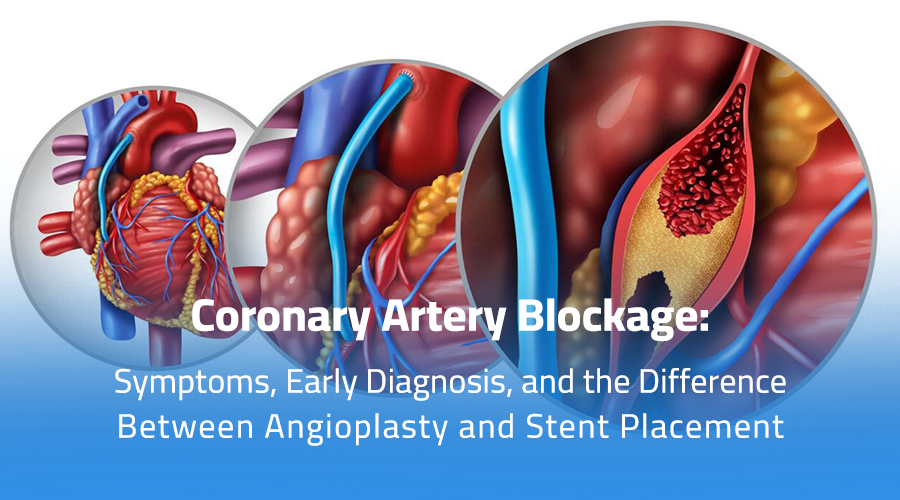
When fatty deposits (called plaques) build up inside these arteries, they narrow gradually, reducing blood flow to the heart.
If blood flow stops completely, it results in a full blockage that can cause a heart attack (myocardial infarction).
Causes of Coronary Artery Blockage
Several factors contribute to artery blockage, including:
- High LDL cholesterol – causes fat buildup on artery walls.
- Smoking – damages blood vessel linings and accelerates plaque formation.
- High blood pressure – strains arteries and weakens their walls over time.
- Diabetes – increases blood viscosity and impairs circulation.
- Obesity and physical inactivity – raise blood lipid levels and reduce blood flow.
- Genetic factors and aging – risk increases in men over 40 and postmenopausal women.
Symptoms of Coronary Artery Blockage
Symptoms often start mild and intermittent but worsen over time.
Common early signs include:
- Chest pain or pressure (angina) – typically felt in the center or left side of the chest, possibly radiating to the arm, shoulder, or jaw. It worsens with exertion and eases with rest.
- Shortness of breath – due to reduced pumping efficiency of the heart.
- Palpitations or irregular heartbeat.
- Unexplained fatigue or weakness – especially in women and the elderly.
- Dizziness or fainting – caused by reduced blood flow to the brain.
- Cold sweat or nausea during exertion – classic sign of ischemia.
Note: Some patients may show subtle or atypical symptoms, making regular check-ups essential—particularly for smokers, diabetics, and hypertensive individuals.
Early Diagnosis of Coronary Artery Blockage
Early detection allows timely intervention before a heart attack occurs.
Diagnostic methods include:
- Electrocardiogram (ECG) – detects abnormalities in heart rhythm or ischemia.
- Exercise stress test – measures heart response during exertion.
- CT Coronary Angiography – visualizes plaques and blockage severity.
- Diagnostic catheterization – involves inserting a thin tube (usually via the groin or wrist) and injecting dye to map the arteries precisely.
- Blood tests – assess cholesterol, triglycerides, and cardiac enzymes.
Treatment of Coronary Artery Blockage
Treatment depends on the blockage severity and overall health condition.
Doctors typically begin with medication, but if that’s insufficient, angioplasty or stent placement may be required.
Difference Between Cardiac Catheterization and Stent Placement
Many patients confuse the two, but they differ significantly in purpose and process.
- Cardiac Catheterization
A minimally invasive diagnostic and therapeutic procedure performed under local anesthesia.
A thin catheter is inserted into an artery to visualize the coronary vessels. The doctor may inflate a balloon to widen a narrowed artery if needed.
Advantages:
- Non-surgical procedure.
- Quick recovery (within hours to a day).
- Useful for both diagnosis and temporary artery dilation.
- Stent Placement
If severe blockage is detected during catheterization, the doctor may insert a stent—a small metallic mesh tube—to keep the artery open.
Types of stents:
- Bare-metal stents (BMS).
- Drug-eluting stents (DES) – release medication to prevent re-narrowing.
Procedure steps:
- Insert the catheter.
- Guide a small balloon to the blockage site.
- Inflate the balloon to widen the artery and place the stent.
- Remove the catheter, leaving the stent to support the artery wall.
Results:
- Immediate blood flow improvement.
- Chest pain relief.
- Reduced risk of future heart attacks.
Medications After Catheterization or Stent Placement
Patients must continue taking prescribed medications to prevent clotting and ensure long-term stent function, such as:
- Aspirin or Clopidogrel.
- Statins (cholesterol-lowering drugs).
- Blood pressure and diabetes medications.
Never stop treatment without consulting your doctor.
Prevention After Treatment
Treatment doesn’t mean full recovery—continuous care is crucial to maintain heart health.
Prevention tips:
- Quit smoking completely.
- Follow a low-fat, low-salt diet.
- Engage in daily physical activity (e.g., 30-minute walks).
- Maintain healthy weight and control blood pressure/sugar.
- Do regular checkups every 6 months.
When to See a Doctor Immediately
- Recurring chest pain after treatment.
- Shortness of breath or rapid heartbeat.
- Dizziness or fainting episodes.
- Pain or swelling at the catheter site.
Any of these symptoms require prompt medical evaluation.
Conclusion
Coronary artery blockage is a serious yet manageable condition with early detection and proper care.
Cardiac catheterization is used for diagnosis and temporary artery dilation, while stent placement ensures long-term blood flow.
Consistent prevention and a healthy lifestyle remain the foundation of strong heart health.
If you experience frequent chest pain or shortness of breath,
Book your consultation now with Dr. Ehab El-Sharkawy,
Assistant Professor of Cardiothoracic Surgery, Faculty of Medicine, Cairo University (Qasr El-Aini),
for early diagnosis and advanced treatment of artery blockages using the latest angioplasty and stent techniques.